


Just $200,000 a year could make a world of difference to the one in every 500 babies born with hydrocephalus in Australia each year. Many more children and adults acquire hydrocephalus as a result of accidents and, left untreated, it can cause severe disability, even death. Yet there is little public awareness of the condition and not enough government funding. Today Fairfax Regional Media is launching a campaign to change all that, but we need your help. We begin with Darcy's story.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
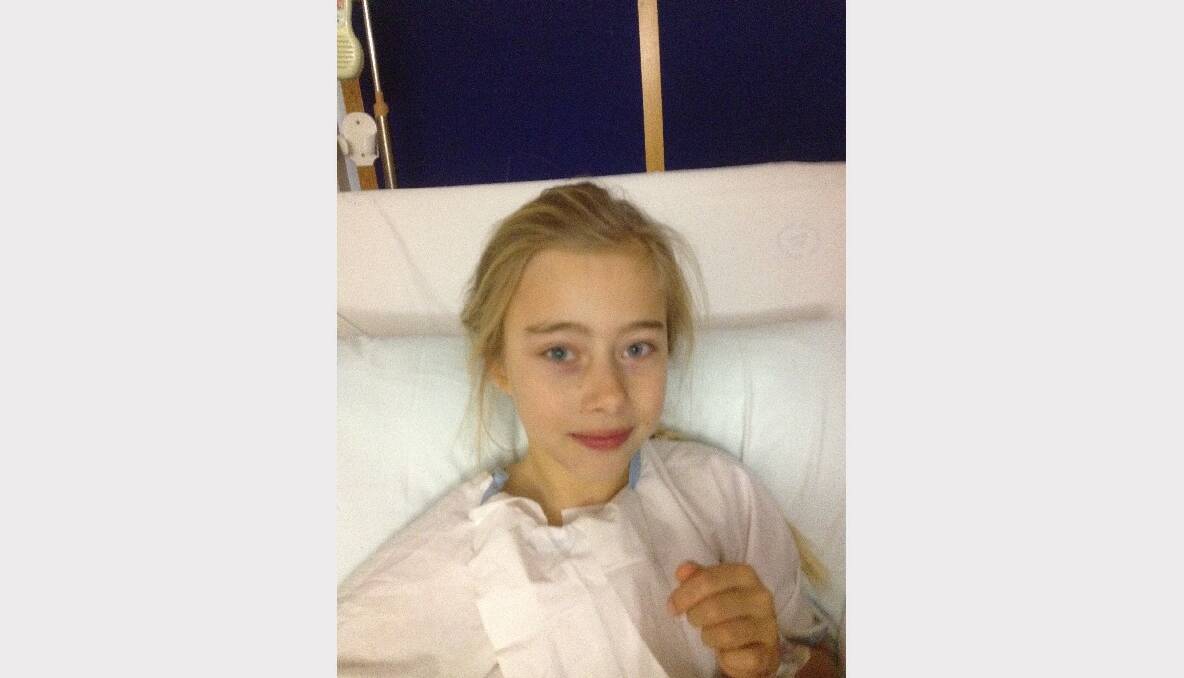
With her long brown legs and mane of golden hair, Darcy Coppin looks the very picture of a happy, healthy Australian child.
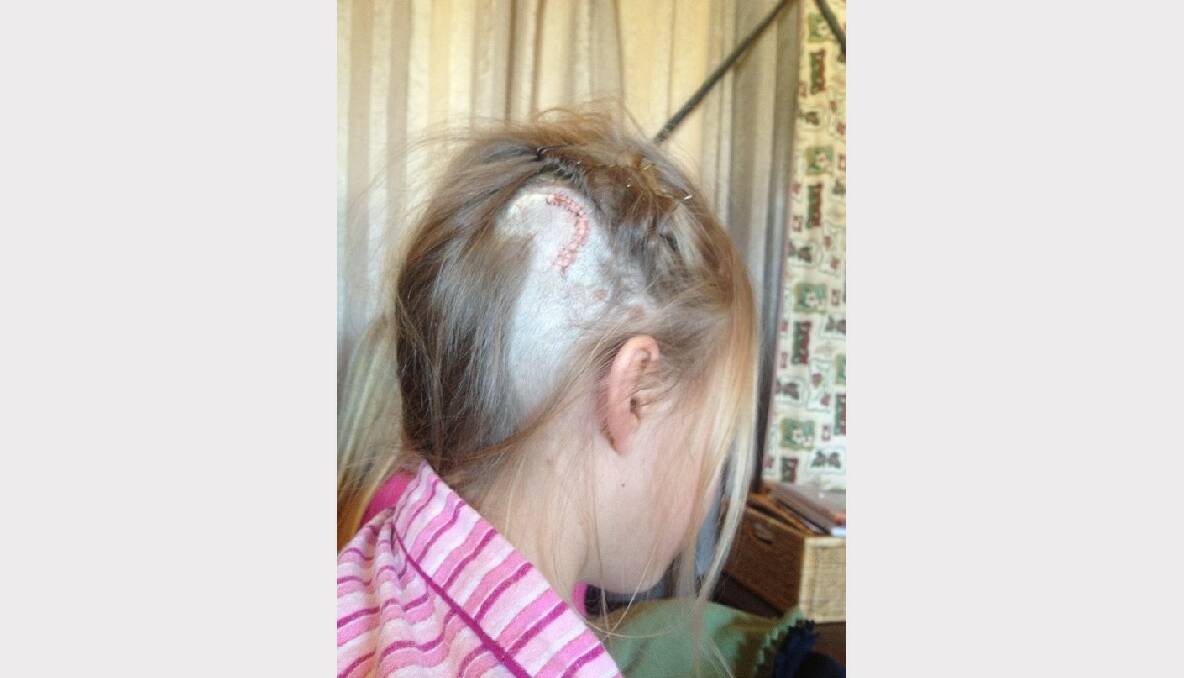
But what's hidden beneath her long blonde locks is a deadly condition that affects one in every 500 Australian babies each year yet is failing to attract even the most meager government funding to help find a cure.
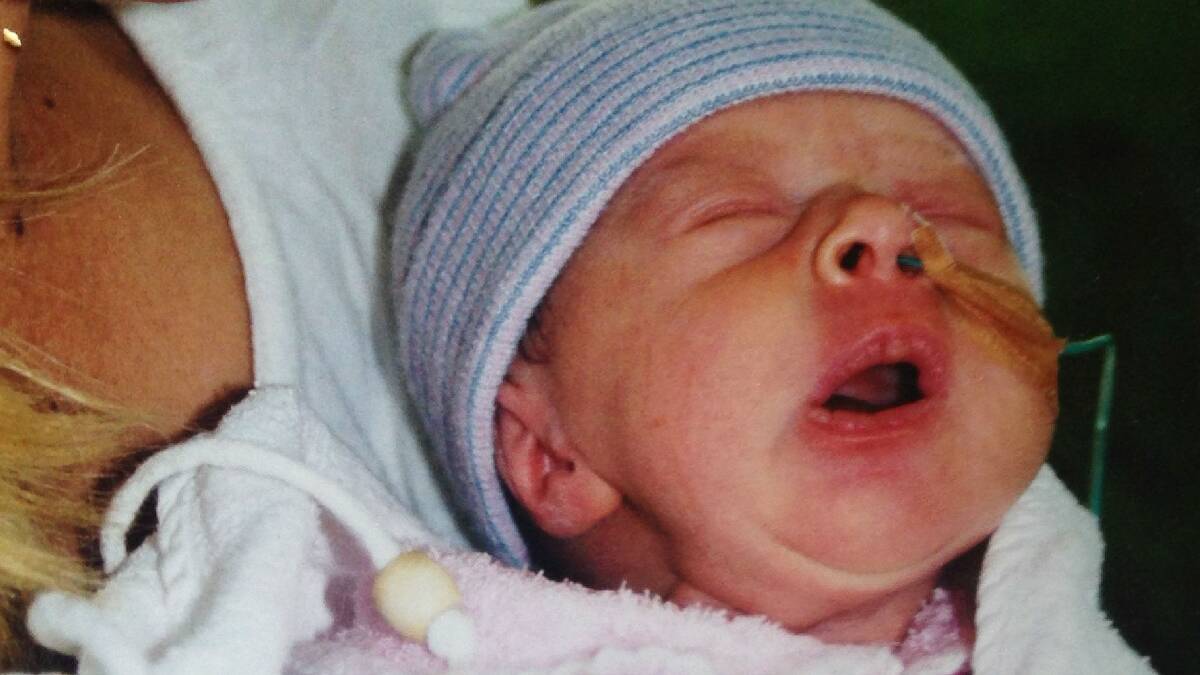
Darcy was born with hydrocephalus - a life-threatening medical condition which, if left untreated, is fatal.
Hydrocephalus occurs when there is an excessive accumulation of cerebro-spinal fluid (CSF) in the brain. It can be congenital or acquired later in life.
It is the most common clinical problem paediatric neurosurgeons face and one of the most common congenital problems in children - twice that of Down syndrome.
The usual treatment is the insertion of a shunt, which drains the fluid from the brain.
The shunt was originally developed by engineer John Holterin the 1960s in a bid to save his own son from what then was a death sentence. It has not changed dramatically since its first use.
The shunt has saved many lives but still has the highest failure rate of any medical implant. Patients are constantly faced with the prospect of shunt malfunction or infection and the only treatment is delicate neurosurgery to fit a replacement.
For children like Darcy and their families, it means living with a ticking timebomb, never knowing if or when the shunt will fail.
Darcy's mum and dad, Jane and Brad Coppin, have moved closer to Moruya Hospital on the NSW South Coast in case the worst happens and are counting their blessings that their 10-year-old is currently so well.
"We've just celebrated her first shunt-aversary since her third shunt was put in," Jane said.
"The last shunt lasted seven years. We've had a really good run - five years is a good run.
"Darcy is living a completely normal life, she's a great case however we know we need to be ready because things can change overnight."
The Coppins are using this small window of respite to put their efforts into raising awareness of hydrocephalus and lobbying for the small amount of annual funding needed to develop better treatment and possibly a cure.
"Early diagnosis leads to better outcomes but too few people know about hydrocephalus. If you think your baby's head is growing too quickly, get it checked out."
- Jane Coppin.
"When you are in crisis, there is no space to think about anyone else," Jane said.
"But we have to do something. Early diagnosis leads to better outcomes but too few people know about hydrocephalus. If you think your baby's head is growing too quickly, get it checked out. It's vital that it is diagnosed before the fontanelle closes."
The second part of the Coppins' mission is to see more research done into shunts and their development.
"The long-term prospects of people living with hydrocephalus are dependent upon the function of their shunt," Jane said.
"Yet at the moment what shunt is used is very much a subjective decision by the surgeon. There is no registry to collate statistical data on what's the best way forward."
One of Australia's leading neurosurgeons, Professor Brian Owler, has been working on the registry proposal for 10 years and has had vocal support from the Coppins.
They say a national registry could compile information on treatment to sort out better methods to preserve quality of life and, in some cases, save life.
It would help prevent much of the dangerous maintenance surgery performed at huge expense to taxpayers and risk to patients.
Professor Owler has now won a $150,000 Federal Government commitment to establish the Shunt Registry, but not the $200,000 recurrent funding needed to actually make it function.
Yet over three years it has cost the Westmead Children's Hospital, conservatively, $1 million a year to implant shunts and another $2.7 million to maintain existing implants, most of that due to infections and blockage - making the $200,000 needed seem like a pittance.
Jane says that seems to be part of the problem.
"The irony is that when Brian (Owler) met Catherine King (then Parliamentary Secretary for Health and Ageing) earlier this year she couldn't believe it was such a small amount.
"If we can improve the type of shunts that we are using we can reduce the infection rate and save hundreds of thousands of dollars each year.
"Fifty per cent of shunts fail in the first two years after insertion, 70 per cent of all shunt operations are replacements, two thirds of patients are affected intellectually, shunt replacement can cause stroke, sufferers may develop epilepsy - seizures can occur as a result of hydrocephalus - and physical limitations and gross motor/coordination problems can occur."
It's not good enough, particularly when young lives as precious as Darcy's are at stake.
Read Jane Coppin's story here >>> Through a mum's eyes

